Monkeypox and "monkey brain"
01.06.2022
Will we have quarantines again? Will we have to be vaccinated against smallpox once more, given that the West's latest generations have grown susceptible to orthopoxviruses? What kind of measures should be used to curb the spread of monkeypox outbreaks among the MSM community and what can we do to ensure that the media refrain from dubbing monkeypox another "gay plague”?
A new shit-storm is sweeping through the Internet, all because those raising the latest alarms about virus-related topics lack any expertises. The comments on monkeypox are being made by people who have no idea which pox they have been vaccinated against, not even understanding that chickenpox is as related to smallpox as a living room chair is to an electric chair. Those who claim to be experts on viruses, tanks, howitzers, even the intricacies of air traffic ground control, claim that the current news about monkeypox is nothing more than the latest attempt to scare people with the threat of another plandemic, calling it "another freak of nature", some even claiming that "this [monkeypox] applies only to members of the gay community who indeed deserve it!". All this means that once again, just as with the coronavirus pandemic, ignorance, misinformation and panic are rampant.
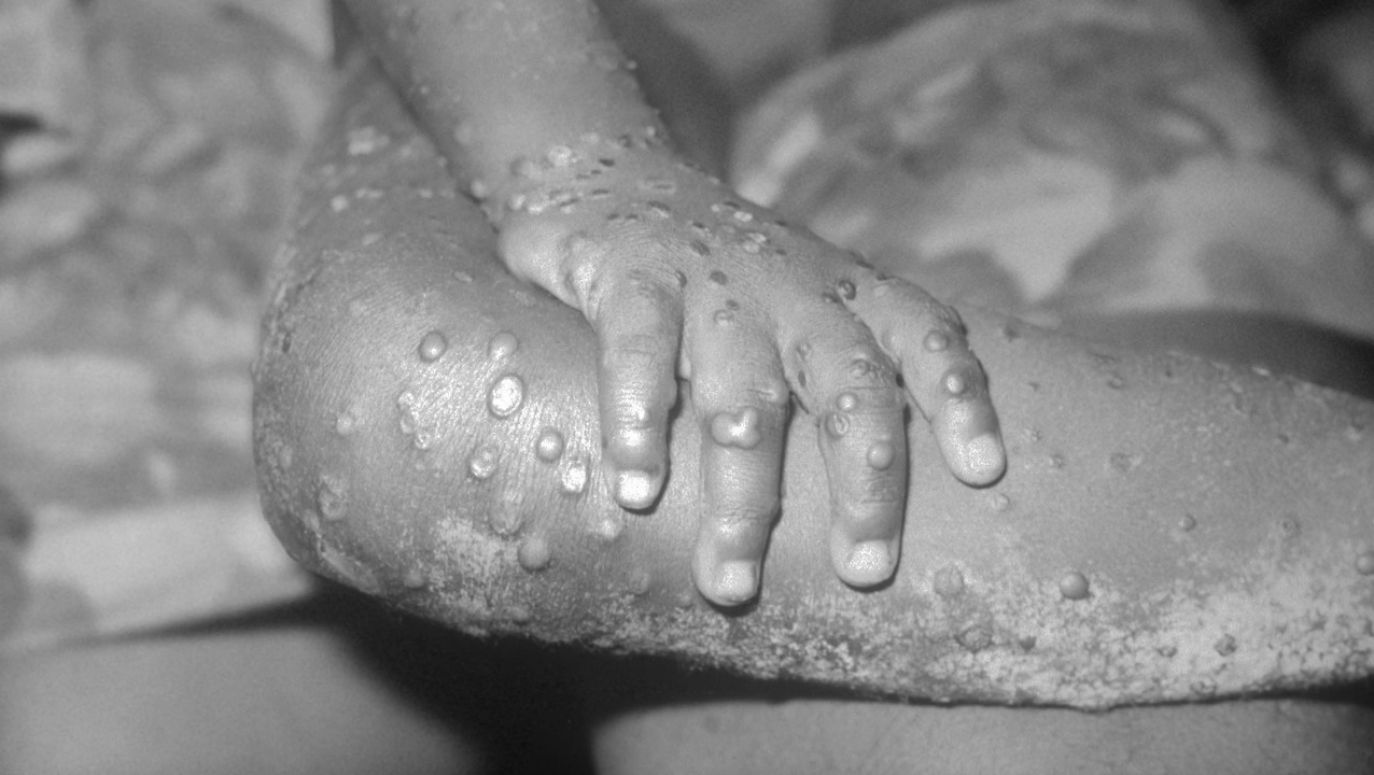
So here is what we should know. Unlike chickenpox, but just like smallpox, monkeypox is caused by a virus from the orthopoxvirus genus. These are viruses with genetic material in the form of DNA, of large size, with approximately 250 genes each (and not just a dozen, as is the case for coronavirus). That monkeypox belongs to the same group as smallpox is good news because the classic smallpox vaccine, created at the end of the 18th century by Edward Jenner on the basis of cowpox virus, that was widely used until the 1980s, is 85 per cent effective against monkeypox.
Therefore, one can safely say that, unlike Covid-19, monkeypox is not a new disease. The virus was initially identified in monkeys imported from Africa by Danish laboratories in 1959. However, the name given to it is misleading since its main carriers are in fact rodents. The first human cases of the disease were recorded in the Democratic Republic of the Congo in 1970. The disease is endemic in both Central Africa, where it is more lethal, as well as West Africa, where a milder variant of the virus is present. Each year in these two regions, some 2,000 highly symptomatic cases of the disease are recorded, with a mortality rate of between 1 and 10 per cent, depending on the variant of the virus, compared to a 30-to-85 per cent lethal rate in case of smallpox. It should be noted that these rates apply to African population groups that can be malnourished and suffering from other diseases, including AIDS.
The first non-African monkeypox epidemic took place around 20 years ago in the US Midwest, where 47 cases were recorded. Those infected had come into very close contact with people who had the misfortune of buying seemingly innocuous rodents that turned out to be virus-infected -- rats believed to have originated from Gabon. Nobody died in the epidemic that was caused by the West African variant of the virus.
Because of this first monkeypox epidemic, since 2019 we have had a vaccine against it, registered in the US, the European Union and in Canada. It prevents the disease even when administered up to four days after a person has been exposed to the virus. It can also provide protection for contacts of suspected or confirmed cases. This is especially useful given the increasing number of wealthy Poles now spending their holidays in exotic locations where tropical diseases (such as monkeypox) can be caught. In this context, it is worth noting that medicines against monkeypox such as tecovirimat and brincidofovir also exist. However, they are not widely available.
Sexually transmitted
Up to now monkeypox has been a classic viral zoonosis, meaning it can "jump” from animals to humans, whereas transmission among humans has been less likely to occur. However, the current epidemic indicates that it is spreading exceptionally fast between people, something that never occured before, even in Africa. Surprisingly, in just a few weeks, the total number of cases is higher than all the non-African cases combined since 1970. And even though we know the so-called index case, i.e. we know exactly who was first diagnosed with the disease (a British male who returned from Nigeria on May 4 and fell sick two days later, diagnosed as a postive case of monkeypox), in no way can we be 100 per cent certain that the entire epidemic, or simply the British wave, started because of him. This is bad news but it shouldn't cause panic.
The current outbreak is a disturbing return of the orthopoxvirus genus to the global spotlight at a time when we had all but forgotten about this threat. The WHO announced that smallpox was globally eradicated in 1980. Will the situation change now? Will quarantines be imposed again on wide circles of those deemed at risk of contact with the sick? Will we be vaccinated again with the oldest vaccine in the world, all because the two latest generations to have grown up in the Western world are susceptible to all orthopoxviruses because this once common prophylaxis was suspended? What kind of measures should be used to curb the spread of monkeypox outbreaks among the MSM community and, at the same time, how do we go about stopping the media from describing monkeypox as another "gay plague”?
The niche left empty by a cousin
All these questions need to be answered soon. Especially since the resources of vaccines available here and now are not large enough, and certainly insufficient to immediately vaccinate the entire global population. Indeed, they are not even sufficient to vaccinate the Western population that missed out on being inoculated against smallpox. However, it is possible that there are sufficient vaccines to protect medical service personnel, especially those in contact with the virus.
Needless to say, the answers to these difficult questions must not be given to us by online dilettantes. They must be provided solely by orthopoxvirus experts. These experts exist and cooperate with each other. According to Wojciech Andrusiewicz, the spokesman of the Polish Ministry of Health, for example, the Polish National Institute of Public Health -- National Institute of Hygiene cooperates with Germany's Robert Koch Institute.
According to scientists, epidemics of this type "generally die by themselves" because many infected people never infect anyone else. However, since the current monkeypox epidemic is geographically widespread, it cannot be ruled out that its spread stems from several independent sources (e.g. the index case in Portugal has nothing to do with the index case in the UK). Moreover, the number of cases in terms of the timeframe seems surprisingly high for non-African conditions. This epidemic is considered "really rare and unusual" so it is thought unlikely that it will become a major threat to the general population and develop along the lines of, for example, COVID-19.
Nonetheless, further questions have to be raised about the need to keep the global population vaccinated against smallpox despite its pronounced eradication since it seems obvious that nature abhors a vacuum. And certainly, it is high time to consider making this vaccine obligatory for travellers going to Africa or introduce compulsory vaccination against monkeypox.